Eczema is a common skin condition that affects millions of people worldwide. It is a chronic inflammatory disorder characterized by red, itchy, and inflamed skin. Understanding the causes, symptoms, and treatments of eczema is crucial for effective management and relief. In this article, we will delve into the various aspects of eczema and provide valuable insights for individuals dealing with this condition.
Tóm tắt nội dung
- 1 What is eczema?
- 2 The underlying causes of eczema
- 3 Recognizing the symptoms of eczema
- 4 Different types of eczema
- 5 How eczema is diagnosed
- 6 Where can you find treatment for eczema?
- 7 FAQs
- 7.0.0.1 Is eczema contagious?
- 7.0.0.2 Can eczema kill you?
- 7.0.0.3 Can eczema be caused by stress?
- 7.0.0.4 Can eczema cause blisters?
- 7.0.0.5 Can eczema cause hair loss?
- 7.0.0.6 Where did eczema come from?
- 7.0.0.7 Does eczema always itch?
- 7.0.0.8 Is eczema an autoimmune disease?
- 7.0.0.9 Should eczema be kept moist or dry?
What is eczema?
Eczema, also known as atopic dermatitis, is a skin condition that causes the skin to become red, inflamed, and itchy. It is often accompanied by dryness, cracking, and oozing of the skin. Eczema can occur at any age, but it is most commonly found in infants and children. The exact cause of eczema is still not fully understood, but it is believed to result from a combination of genetic and environmental factors.

Defining eczema
At its core, eczema is an inflammatory skin condition that manifests itself through various symptoms. The immune system in individuals with eczema reacts abnormally to triggers, leading to inflammation and irritation of the skin. This can cause discomfort and impact the quality of life for those affected.
When it comes to understanding eczema, it’s important to consider the different types of the condition. There are several subtypes of eczema, including atopic dermatitis, contact dermatitis, nummular eczema, and dyshidrotic eczema. Each subtype has its own unique characteristics and triggers, further emphasizing the complexity of this skin condition.
One of the key features of eczema is its chronic nature. Eczema flare-ups can come and go, with periods of remission and exacerbation. This unpredictability can make it challenging for individuals with eczema to manage their symptoms effectively.
Prevalence of eczema
Eczema is a prevalent condition, affecting around 10-20% of infants and around 3% of adults worldwide. It is more commonly found in developed countries, with urban environments and specific genetic profiles playing a role in its prevalence.
Research has shown that certain genetic variations can increase the risk of developing eczema. For example, mutations in the filaggrin gene have been associated with an increased susceptibility to eczema. Additionally, environmental factors such as exposure to allergens, pollutants, and certain lifestyle choices can contribute to the development and severity of eczema.
It’s worth noting that eczema can have a significant impact on the quality of life for those affected. The constant itching, discomfort, and visible skin changes can lead to sleep disturbances, psychological distress, and social isolation. Managing eczema requires a multidimensional approach that addresses both the physical and emotional aspects of the condition.
While there is currently no cure for eczema, various treatment options are available to help manage symptoms and improve quality of life. These can include topical creams, oral medications, phototherapy, and lifestyle modifications. It is important for individuals with eczema to work closely with healthcare professionals to develop a personalized treatment plan that addresses their specific needs and triggers.
In conclusion, eczema is a complex and chronic skin condition that affects millions of people worldwide. Understanding its defining characteristics, prevalence, and impact on individuals is crucial in providing effective support and management strategies for those living with eczema.
The underlying causes of eczema
While the exact cause of eczema remains unknown, researchers have identified several factors that contribute to its development.
Eczema, also known as atopic dermatitis, is a chronic inflammatory skin condition that affects millions of people worldwide. It is characterized by red, itchy, and inflamed skin patches that can be both uncomfortable and unsightly. Understanding the underlying causes of eczema is crucial for effective management and treatment.
Genetic factors
Eczema tends to run in families, indicating a genetic component. Certain gene variations have been associated with an increased risk of developing eczema, although the specific genes involved are still being investigated. These genetic factors can influence the skin’s barrier function, immune response, and overall susceptibility to inflammation.
Moreover, research suggests that individuals with a family history of eczema may have a higher likelihood of developing other allergic conditions, such as asthma and hay fever. This further highlights the role of genetics in the development of eczema and its association with other allergic diseases.
Environmental triggers
Environmental factors can play a significant role in triggering eczema flare-ups. These triggers can vary from person to person, making it important for individuals to identify and avoid their specific triggers.
Exposure to allergens is a common environmental trigger for eczema. Allergens such as pollen, pet dander, and dust mites can cause an immune response in susceptible individuals, leading to inflammation and eczema symptoms. Additionally, irritants like harsh soaps, detergents, and certain fabrics can disrupt the skin’s barrier function and trigger flare-ups.
Furthermore, changes in weather and humidity levels can impact eczema symptoms. Cold and dry weather can cause the skin to become more prone to dryness and irritation, while hot and humid conditions can lead to excessive sweating and increased itchiness. Stress is another environmental trigger that can exacerbate eczema symptoms, as it can disrupt the immune system and trigger inflammatory responses.
It is important to note that while these factors contribute to the development and exacerbation of eczema, they may not be the sole cause. Eczema is a complex condition influenced by a combination of genetic, environmental, and immune factors. Ongoing research aims to further unravel the underlying mechanisms of eczema, paving the way for improved treatments and management strategies.
Recognizing the symptoms of eczema
Eczema can present with a range of physical signs and may also have emotional and psychological implications for individuals experiencing it. Understanding the symptoms and their impact is crucial for effective management and support.
Common physical signs
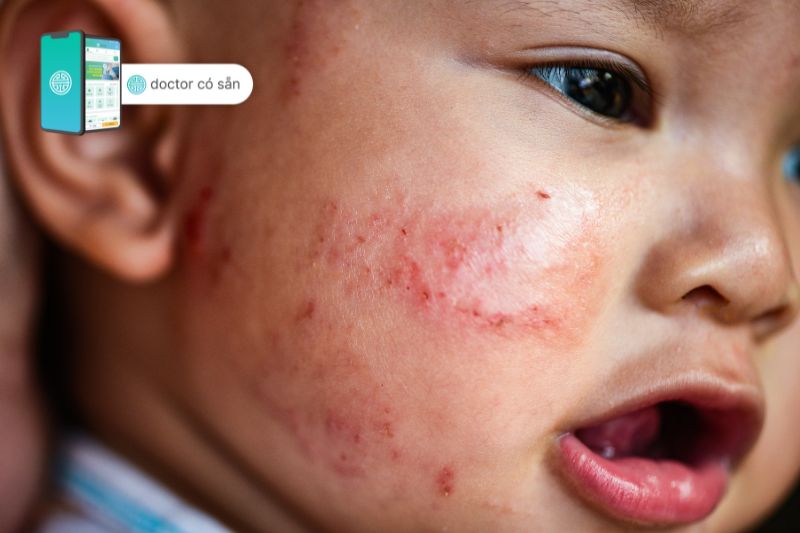
The physical signs of eczema include redness, itching, dryness, and inflammation of the skin. These symptoms can range from mild to severe, depending on the individual and the specific type of eczema they have.
In mild cases, the skin may appear slightly red and feel itchy. It may also feel dry and rough to the touch. As the condition progresses, the skin may become more inflamed, leading to increased redness and itching. In severe cases, the skin may develop blisters, crusting, or scaling, which can cause significant discomfort and pain.
While eczema can affect various areas of the body, certain areas are more commonly affected. These include the face, hands, feet, and inside the elbows and knees. The skin in these areas is more sensitive and prone to irritation, making them more susceptible to eczema flare-ups.

Emotional and Psychological Impact
Eczema can have a profound impact on an individual’s emotional and psychological well-being. The persistent itching, discomfort, and visible skin changes can lead to feelings of self-consciousness, embarrassment, and even depression.
Living with eczema can be challenging, as individuals may feel the need to constantly hide their affected skin or avoid social situations altogether. The visible signs of eczema can attract unwanted attention and may result in negative judgments or misconceptions from others.
Furthermore, the constant itching and discomfort can disrupt sleep patterns, leading to fatigue and irritability. The physical symptoms of eczema can also affect daily activities, such as work or school, causing additional stress and frustration.
It is essential to address these aspects of eczema along with the physical symptoms to ensure holistic management of the condition. This may involve seeking emotional support, practicing stress-reducing techniques, and developing coping strategies to improve overall well-being.
By understanding the full impact of eczema, both physically and emotionally, individuals can take proactive steps to manage their condition effectively and improve their quality of life.
Different types of eczema
Eczema, a common skin condition, can manifest in various forms, each with its unique characteristics and triggers. Understanding the different types of eczema can help individuals manage and treat their symptoms effectively.
Atopic dermatitis
Atopic dermatitis is the most common form of eczema, affecting millions of people worldwide. It often starts in childhood and can persist into adulthood. This chronic condition is characterized by dry, itchy skin that can become inflamed and irritated. Individuals with atopic dermatitis may experience flare-ups triggered by various factors, including allergens, stress, and environmental factors.
Research suggests that atopic dermatitis is influenced by both genetic and environmental factors. Individuals with a family history of eczema, asthma, or hay fever are more likely to develop atopic dermatitis. Additionally, certain environmental factors, such as exposure to harsh chemicals or extreme weather conditions, can exacerbate symptoms.
Contact dermatitis
Contact dermatitis occurs when the skin comes into direct contact with an irritant or allergen. This type of eczema can lead to a localized rash, redness, and itching. The irritants or allergens responsible for contact dermatitis can vary widely, including certain chemicals, metals, cosmetics, fragrances, and even fabrics.
Individuals who work in occupations that involve frequent exposure to irritants, such as hairdressers, healthcare workers, or construction workers, are at a higher risk of developing contact dermatitis. Additionally, individuals with a history of allergies or sensitive skin may be more prone to this form of eczema.
Dyshidrotic eczema
Dyshidrotic eczema, also known as pompholyx, primarily affects the hands and feet. It is characterized by the formation of small, itchy blisters on the palms, soles, and sides of the fingers and toes. These blisters can be painful and may cause discomfort during everyday activities.
The exact cause of dyshidrotic eczema is unknown, but it is believed to be a combination of genetic and environmental factors. Stress, allergens, and exposure to moist environments, such as excessive sweating or prolonged contact with water, can trigger flare-ups.
Individuals with dyshidrotic eczema may find relief by avoiding triggers, keeping their hands and feet dry, and using moisturizers to prevent excessive dryness.
By understanding the different types of eczema and their triggers, individuals can work with healthcare professionals to develop personalized treatment plans. It is important to note that eczema is a chronic condition, and while there is no cure, proper management can help alleviate symptoms and improve quality of life.
How eczema is diagnosed
Diagnosing eczema involves a comprehensive evaluation of an individual’s medical history, physical examination, and potentially specific tests to confirm the diagnosis.
Medical history evaluation
A detailed medical history can provide valuable insights into an individual’s symptoms, triggers, and family history of eczema or other allergic conditions. This information assists healthcare professionals in making an accurate diagnosis and developing an appropriate treatment plan.
Physical Examination
A physical examination is performed to assess the severity and distribution of the eczema rash. The healthcare provider will examine the skin, noting any redness, swelling, or other characteristic signs of eczema. They may also inquire about any other accompanying symptoms, such as itching or pain.

Skin Tests
In some cases, skin tests may be performed to identify specific allergens that may be triggering or exacerbating the eczema. These tests can involve applying small amounts of suspected allergens to the skin and observing for any reactions.
Where can you find treatment for eczema?
Dr. Michael’s Psoriasis & Skin Clinic leads in dermatology, specializing in complex skin conditions. Their mission focuses on effectively managing Psoriasis, Eczema, Vitiligo, and Fungal Skin Diseases.
Their success stems from Dr. Michael Tirant, PhD, and his three-decade journey refining “Dr. Michael’s method,” supported by esteemed dermatology professors. These standards have gained global recognition, influencing healthcare systems worldwide.
They prioritize safety and efficacy, utilizing premium natural herbs aligned with Dr. Michael’s method. Their treatments, validated through a decade of clinical trials across multiple countries, achieve an impressive 90% effectiveness, even for children and expectant mothers.
Book an appointment today to explore outstanding skincare at Dr. Michael’s Psoriasis & Skin Clinic.

FAQs
Is eczema contagious?
No, eczema is not contagious. It is a non-communicable skin condition and cannot be spread from person to person through direct contact.
Can eczema kill you?
Generally, eczema itself is not life-threatening. However, severe cases of eczema can lead to complications, and in rare instances, infections related to eczema can be serious. It’s essential to manage and treat eczema properly to prevent complications.
Can eczema be caused by stress?
Stress can trigger or exacerbate eczema flare-ups in some individuals. While stress is not a direct cause of eczema, managing stress can be an important part of managing the condition.
Can eczema cause blisters?
Yes, eczema can cause blisters in some cases. This is more commonly seen in a specific type of eczema called “dyshidrotic eczema” or “pompholyx eczema,” which is characterized by small, itchy blisters on the palms of the hands and soles of the feet.
Can eczema cause hair loss?
Eczema itself does not typically cause hair loss. However, scratching the affected areas vigorously can lead to hair loss in those areas due to physical damage to the hair follicles.
Where did eczema come from?
Eczema is not a recent development; it has likely existed for centuries. It is a complex skin condition with genetic and environmental factors contributing to its development.
Does eczema always itch?
Itching is a common symptom of eczema, but not everyone with eczema experiences itching. The severity of itching can vary from person to person and may even vary within the same individual over time.
Is eczema an autoimmune disease?
Eczema is not classified as an autoimmune disease. It is primarily considered a chronic inflammatory skin condition. Autoimmune diseases involve the immune system attacking healthy cells or tissues, which is not the case in eczema.
Should eczema be kept moist or dry?
The general recommendation for managing eczema is to keep the skin moisturized. Dry skin can exacerbate eczema symptoms. Applying moisturizers can help soothe and hydrate the skin, but it’s essential to choose hypoallergenic and fragrance-free products.
Understanding eczema is essential for effective management and treatment. By recognizing the causes, symptoms, and various types of eczema, individuals can take appropriate measures to mitigate flare-ups and improve their overall well-being.
Seeking medical advice and following a personalized treatment plan are crucial for individuals dealing with eczema. With proper care and support, eczema can be managed, allowing individuals to lead a comfortable and fulfilling life.




